Based on these assumptions, it was argued that medical incapacitation should result in a fatal accident no more often than 1 in 1000 million flying hours (1 in 10 9). Further, it was argued that aircrew, as part of the overall aircraft system, should not contribute more than 10% to total risk, and that pilot medical incapacitation should account for only 10% of crew failures. For assessing medical risk, the Workshop decided on a target of 0.1 fatal accidents per 1 million flying hours (1 in 10 7 flying hours). 5 At that time, the all-cause accident rate for commercial airlines was approximately 0.2 per 1 million flying hours. 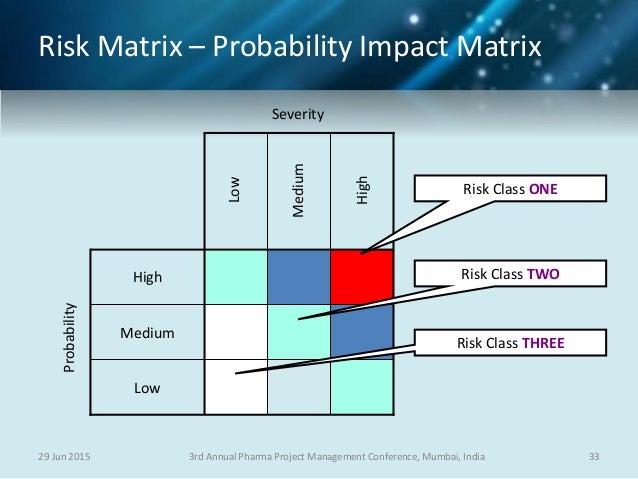
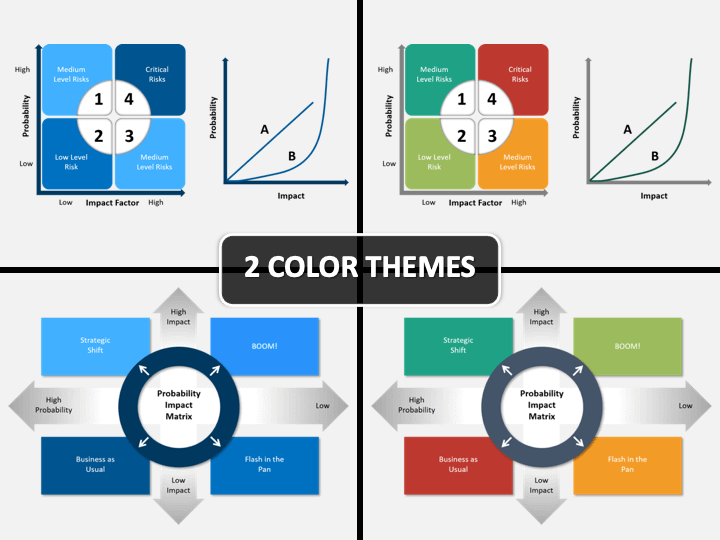
This concept was further developed in the UK at the first UK Workshop in Aviation Cardiology, at which Tunstall-Pedoe proposed what became the ‘1% rule’. In 1973, Ian Anderson (a British physician who had joined the Royal Canadian Air Force (RCAF) and subsequently became the Director of Civil Aviation Medicine in Canada) presented a paper at the 44th Annual Scientific Meeting of the Aerospace Medical Association, in which he proposed that in assessing aeromedical risk for aircrew with medical conditions, aeromedical physicians should attempt to approximate the accepted aeronautical airworthiness risk accepted by aeronautical engineers for fatal accidents, which at that time was 1 in 10 million (10 7) flying hours. Restrictions were often determined by a board of aeromedical specialists, generally comprising experienced clinicians who based their decisions on their clinical experience with such conditions. Civilian aircrew were considered for limited medical certificates under a process involving accredited medical conclusion, relevant ability, skill and experience, and possible licence endorsement with special limitations, as laid out in International Civil Aviation Organization Annex 1. Over time, the excessive loss of experienced aircrew, secondary to their medical conditions, led to the development of specific conditions under which such aircrew might be returned to at least restricted flight duties (often formally drafted as waivers in a waiver guide). Aircrew who developed medical conditions that did not meet medical standards were generally removed from duty. Aeromedical standards evolved to select out individuals with conditions considered likely to cause incapacitation, and while these became increasingly rigid, they often had little or no supportive evidence to justify them (examples include the Schneider index 2 (US Army Air Corps), the physical efficiency index 3 (Royal Air Force) and, later, anomalies on the electroencephalogram). 1Įarly aviation medicine specialists primarily focused on the special senses, and protection of the aviator from environmental factors such as hypothermia, hypoxia and sustained acceleration. Aircraft accident rates steadily declined, and modern aircrafts have a very low risk of mechanical or systems failure. Early fliers were primarily concerned about the risk of mechanical failure, but, over time, engineers improved aircraft design and construction so that other factors became increasingly important, including weather, pilot judgement and pilot health. Risk assessment is an integral component of aviation safety whether for private recreational flying or major airline operations, an assessment of risk forms part of every aircraft flight. This manuscript describes an approach to aeromedical risk management which incorporates risk matrices and how they can be used in aeromedical decision-making, while highlighting some of their shortcomings. Risk assessment is often visualised as a risk matrix, with the level of risk, urgency or action required defined for each cell, and colour-coded as red, amber or green depending on the overall combination of risk and consequence. Risk management has subsequently evolved as a formal discipline, incorporating risk assessment as an integral part of the process. 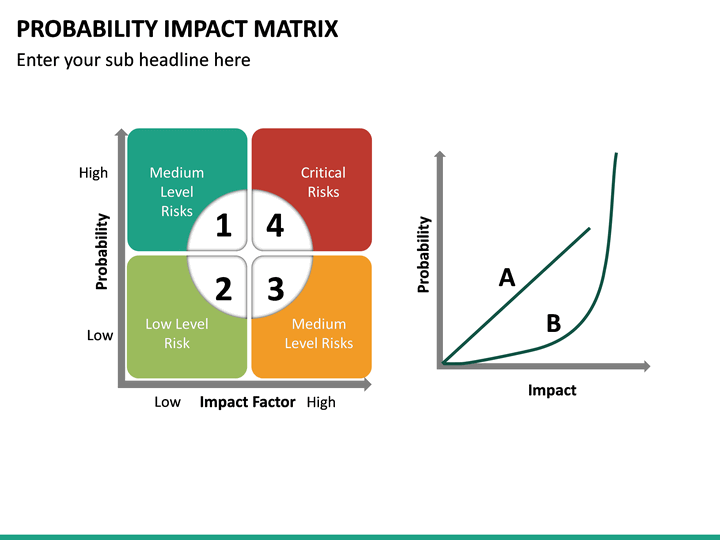
The concept of considering aeromedical risk as part of the spectrum of risks that could lead to aircraft accidents (including mechanical risks and human factors) was first proposed in the 1980s and led to the development of the 1% rule which defines the maximum acceptable risk for an incapacitating medical event as 1% per year (or 1 in 100 person-years) to align with acceptable overall risk in aviation operations. Was based on aeromedical standards designed to eliminate individualsįrom air operations with any identifiable medical risk, and led to frequent medical disqualification. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
